Contents
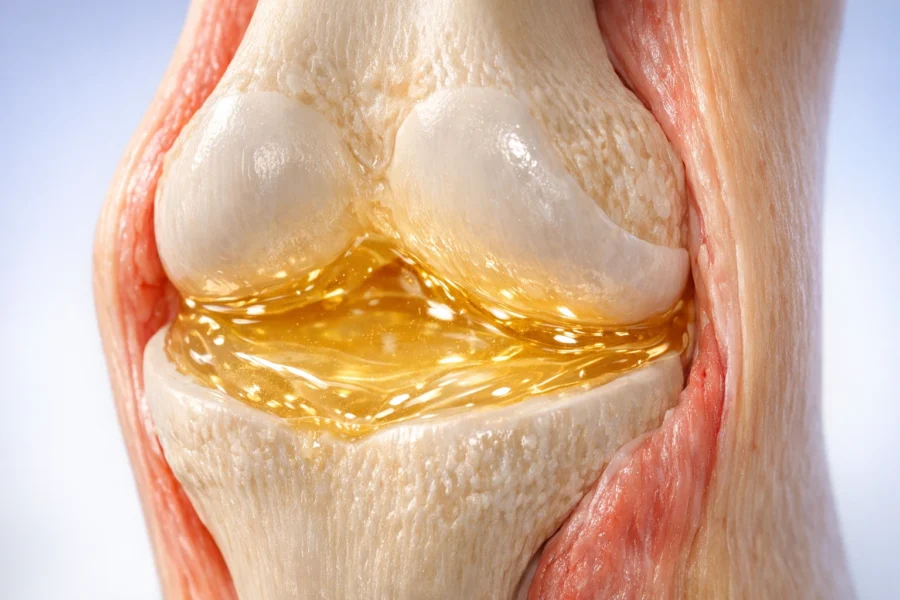
Your joints move thousands of times a day without grinding themselves to dust. Synovial fluid is the reason why. This viscous, pale-yellow liquid sits inside your movable joints, acting as a lubricant, shock absorber, and nutrient delivery system all at once.
What Synovial Fluid Actually Is
Synovial fluid, also called synovia, is a non-Newtonian fluid found in the cavities of synovial joints, which are the most common joint type in the human body. Knees, hips, shoulders, and knuckles all rely on it. The Cleveland Clinic describes it simply: synovial fluid “reduces friction and helps your joints move smoothly like they should.”
What makes it non-Newtonian is genuinely interesting. Unlike water, which flows at a constant rate, synovial fluid changes viscosity depending on applied force. Under high-speed or high-load movement, it thins out and flows more freely, protecting joints during both slow stretches and explosive sprints. Think of cornstarch mixed with water: it resists sudden force but yields under gentle pressure.
A healthy large joint like the knee contains only about 0.5 to 4 mL of this fluid. That is less than a teaspoon, yet it does an enormous amount of work.
Composition: What It’s Made Of
Synovial fluid starts as an ultrafiltrate of blood plasma, then gets enriched by the synovial membrane lining the joint capsule. The two key molecules driving its function are hyaluronic acid and lubricin.
Healthy joints maintain a hyaluronic acid concentration of roughly 3 to 4 mg/mL, with molecular chains weighing approximately 6 to 7 million Daltons. That high molecular weight gives the fluid its thick, gel-like consistency. In osteoarthritic joints, inflammation breaks those long chains into shorter fragments, reducing viscosity at precisely the moment joints need lubrication most.
Lubricin (proteoglycan 4) handles surface-to-surface lubrication between cartilage layers. White blood cells are also present, but in very small numbers: normal fluid contains fewer than 200 cells per microliter. When that count climbs above 2,000, it signals inflammation; above 50,000 points to a serious joint infection.
The Four Core Functions
As Physiopedia’s overview of synovial fluid explains, this fluid does far more than reduce friction. Here is how each function works mechanically:
Lubrication: Hyaluronic acid and lubricin form a slippery film between cartilage surfaces, preventing bone-on-bone contact during movement.
Shock Absorption: The fluid’s viscosity distributes compressive forces across the joint, cushioning impact during walking, running, or lifting.
Nutrient Delivery: Cartilage is completely avascular, meaning it has no blood supply of its own. Synovial fluid is the sole source of oxygen and glucose for chondrocytes, the cells that maintain cartilage.
Waste Removal: The same diffusion process that delivers nutrients carries metabolic waste products back out of cartilage tissue.
How Synovial Fluid Changes With Disease
When joints become diseased or injured, synovial fluid changes in measurable ways. Clinicians use a procedure called arthrocentesis (joint aspiration) to draw fluid from a joint and analyze it, helping identify the underlying condition.
Normal fluid is clear and pale yellow. Osteoarthritic fluid tends to be slightly cloudy with reduced viscosity, while rheumatoid arthritis produces more inflammatory fluid with elevated white blood cell counts between 2,000 and 75,000 cells per microliter. Septic or infectious arthritis produces thick, opaque fluid with WBC counts exceeding 50,000, requiring urgent treatment.
Understanding how synovial fluid supports joint function in conditions like arthritis helps explain why treatments like viscosupplementation aim to restore the fluid’s lost properties rather than simply masking pain.
Supporting Healthy Synovial Fluid
Lifestyle choices directly influence fluid quality and quantity. Regular, low-impact movement stimulates fluid circulation through the joint, while chronic dehydration can compromise fluid volume since synovial fluid is largely water-based.
Nutrition plays a supporting role as well. Consider these key contributors to joint fluid health:
- Omega-3 fatty acids help reduce joint inflammation, preserving hyaluronic acid chain integrity
- Glucosamine and collagen-rich foods may support the synovial membrane’s ability to produce fluid, though evidence varies
- Consistent hydration keeps fluid volume stable and supports nutrient diffusion into cartilage
- Regular low-impact activity, such as walking or swimming, keeps fluid circulating through the joint
Prolonged inactivity is one of the biggest threats to joint health. Joints that rarely move produce less fluid and circulate it poorly, gradually accelerating cartilage degradation over time.
Does cracking your knuckles damage synovial fluid?
No. The popping sound comes from gas bubbles collapsing within the joint cavity, not from fluid breakdown. Research has not linked knuckle cracking to arthritis or long-term joint damage.
Can you naturally rebuild lost synovial fluid?
The synovial membrane continuously produces fluid, so mild depletion can recover with rest, hydration, and movement. Severe depletion related to disease typically requires medical treatment, including viscosupplementation using artificial synovial fluid for conditions like knee osteoarthritis.
How do doctors analyze synovial fluid?
A physician uses a needle to withdraw fluid from the joint, then evaluates its color, clarity, viscosity, and white blood cell count. Results help distinguish between non-inflammatory conditions, autoimmune diseases, crystal-induced arthritis like gout, and joint infections.